Newsletter Apr2026. The Impact of Stress on Fertility and Hormone Balance
Did you know that stress can directly impact your fertility?
Your body is constantly making decisions about where to allocate energy. When stress is high, it prioritizes survival over reproduction. This shift is controlled by two key systems in the brain: the hypothalamic–pituitary–adrenal (HPA) axis and the hypothalamic–pituitary–gonadal (HPG) axis.
Under chronic stress, the HPA axis increases production of cortisol, your primary stress hormone. At the same time, the HPG axis downregulates reproductive hormones such as progesterone and testosterone (1,2). In simple terms, your body is saying, “Now is not a safe time to reproduce.
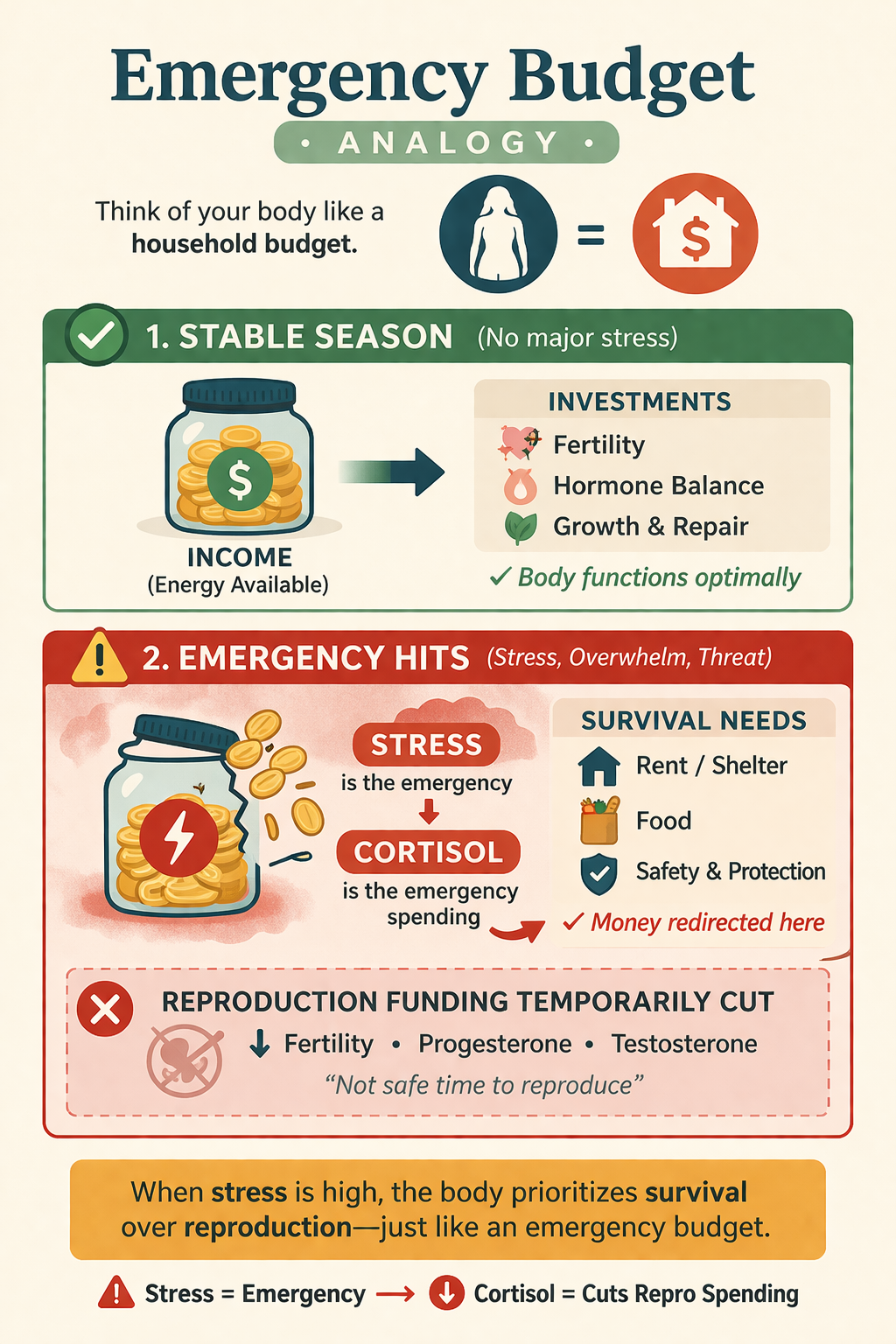
“Emergency Budget” Analogy
Think of your body like a household budget. When everything is stable, you can spend on long-term investments like fertility, hormone balance, and growth. But when an emergency hits, like a big unexpected expense, you shift all your money toward survival needs like rent, food, and safety.
Stress is that emergency.
Cortisol is the emergency spending.
So your body temporarily “cuts funding” to reproduction because it is not essential for immediate survival.
How Stress Disrupts Progesterone and Your Cycle
Progesterone plays a critical role in regulating mood, sleep, and the menstrual cycle. It is often called the “calming hormone” because of its effects on the nervous system.
When stress is chronic, the body shifts hormone production toward cortisol. Both cortisol and progesterone are made from shared precursors derived from cholesterol. While the idea of a “pregnenolone steal” is an oversimplification, research supports that stress can shift steroid hormone production away from reproductive pathways (3).
This can lead to:
A shortened luteal phase
Increased anxiety
Poor sleep
Light or irregular periods
At the same time, estrogen is not suppressed in the same way. However, stress-related habits such as poor diet, gut dysfunction, and toxin exposure can impair estrogen metabolism. This may create a state of relative estrogen dominance, contributing to:
Mood swings and irritability
Breast tenderness
Bloating
Premenstrual symptoms
Cortisol, Testosterone, and Ovulation
Stress also affects testosterone, which is important for both men and women. Testosterone supports libido, energy, muscle mass, and ovulation.
Elevated cortisol suppresses reproductive signaling at multiple levels. It reduces the release of gonadotropin-releasing hormone (GnRH) from the hypothalamus and lowers luteinizing hormone (LH) and follicle-stimulating hormone (FSH) from the pituitary (4). This results in decreased testosterone production.
In women, this disruption can impair ovulation, leading to irregular cycles or missed periods. In more severe cases, this pattern is seen in hypothalamic amenorrhea.
Sleep plays a critical role here as well. High cortisol levels, especially at night, disrupt sleep. Poor sleep then further reduces testosterone production and worsens metabolic health, creating a cycle that is difficult to break.
The Blood Sugar and Hormone Connection
Stress does not just affect hormones directly. It also impacts metabolism.
Cortisol raises blood sugar levels to provide quick energy during stress. Over time, this can contribute to insulin resistance (5). Elevated insulin has several important effects on hormone balance:
It stimulates the ovaries to produce more androgens, including testosterone
It lowers sex hormone-binding globulin (SHBG), a protein that binds testosterone in the bloodstream
Lower SHBG increases the amount of free, active testosterone
This pattern is commonly seen in Polycystic Ovary Syndrome, but it can also occur in women without a formal diagnosis.
Stress, Inflammation, and Estrogen Imbalance
Chronic stress is also associated with increased abdominal fat and low-grade inflammation. Fat tissue is hormonally active and contains an enzyme called aromatase, which converts testosterone into estrogen (6).
At the same time, insulin continues to drive androgen production. The result is a mixed hormonal picture, where both estrogen and testosterone are dysregulated.
This can lead to symptoms such as:
Acne and oily skin
Facial hair growth
Thinning hair at the crown
Heavy or painful periods
PMS and mood swings
Weight gain, especially around the abdomen
Blood sugar crashes and cravings
Rather than a single hormone being “too high” or “too low,” the issue is often a breakdown in communication between systems.
How to Support Stress and Restore Hormone Balance
The good news is that these patterns are often reversible with the right support. The goal is to regulate the stress response, stabilize metabolism, and restore hormonal signaling.
Prioritize Sleep
Sleep is one of the most powerful tools for hormone balance.
Aim for 7 to 9 hours per night
Get sunlight within 30 minutes of waking
Limit screens 60 to 90 minutes before bed
Deep sleep supports cortisol regulation, insulin sensitivity, and reproductive hormone production.
Stabilize Blood Sugar
Balanced blood sugar reduces cortisol spikes and supports hormone health.
Eat protein and healthy fats at each meal
Avoid skipping meals when stressed
Limit caffeine on an empty stomach
Reduce large swings in sugar intake
Exercise with Intention
Exercise is beneficial, but more is not always better.
Strength train 2 to 4 times per week
Incorporate walking or low-intensity movement daily
Avoid excessive high-intensity workouts
For cycling women, consider aligning workouts with your cycle:
Higher intensity in the follicular phase
Lower intensity in the luteal phase
Regulate the Nervous System
Daily stress management helps shift the body out of survival mode.
Breathwork, meditation, or prayer
Journaling
Setting boundaries to reduce chronic stress load
These practices activate the parasympathetic nervous system, which supports healing and hormone balance.
Consider Targeted Supplements
Certain supplements can support stress resilience and hormone regulation:
Ashwagandha may help lower cortisol and support reproductive hormones (7)
Magnesium supports sleep, nervous system regulation, and insulin sensitivity (8)
Inositol improves insulin signaling, supports ovulation, and reduces excess androgens in PCOS (9)
Stress does not just affect how you feel. It changes how your body functions.
By prioritizing survival, chronic stress suppresses reproductive hormones, disrupts ovulation, and alters metabolism. Over time, this can lead to symptoms that affect fertility, energy, mood, and overall health.
The encouraging part is that your body is adaptable. With the right lifestyle changes and targeted support, it is possible to restore balance, improve hormone function, and support fertility naturally.
References
Viau, V. (2002). Functional cross-talk between the hypothalamic–pituitary–gonadal and –adrenal axes. Journal of Neuroendocrinology, 14(6), 506–513. https://doi.org/10.1046/j.1365-2826.2002.00798.x
Whirledge, S., & Cidlowski, J. A. (2010). Glucocorticoids, stress, and fertility. Minerva Endocrinologica, 35(2), 109–125.
Miller, W. L., & Auchus, R. J. (2011). The molecular biology, biochemistry, and physiology of human steroidogenesis and its disorders. Endocrine Reviews, 32(1), 81–151. https://doi.org/10.1210/er.2010-0013
Tilbrook, A. J., Turner, A. I., & Clarke, I. J. (2000). Effects of stress on reproduction in non-rodent mammals: The role of glucocorticoids and sex differences. Reviews of Reproduction, 5(2), 105–113. https://doi.org/10.1530/ror.0.0050105
Joseph, J. J., & Golden, S. H. (2017). Cortisol dysregulation: The bidirectional link between stress, depression, and type 2 diabetes mellitus. Annals of the New York Academy of Sciences, 1391(1), 20–34. https://doi.org/10.1111/nyas.13217
Simpson, E. R. (2003). Sources of estrogen and their importance. The Journal of Steroid Biochemistry and Molecular Biology, 86(3–5), 225–230. https://doi.org/10.1016/S0960-0760(03)00360-1
Lopresti, A. L., Smith, S. J., Malvi, H., & Kodgule, R. (2019). An investigation into the stress-relieving and pharmacological actions of an ashwagandha (Withania somnifera) extract: A randomized, double-blind, placebo-controlled study. Medicine, 98(37), e17186. https://doi.org/10.1097/MD.0000000000017186
Boyle, N. B., Lawton, C., & Dye, L. (2017). The effects of magnesium supplementation on subjective anxiety and stress—a systematic review. Nutrients, 9(5), 429. https://doi.org/10.3390/nu9050429
Unfer, V., Carlomagno, G., Dante, G., & Facchinetti, F. (2012). Effects of myo-inositol in women with PCOS: A systematic review of randomized controlled trials. Gynecological Endocrinology, 28(7), 509–515. https://doi.org/10.3109/09513590.2011.650660
Disclaimer - This document is for informational purposes only and is not intended to provide medical advice, diagnosis, or treatment. Always consult with a qualified healthcare professional before making any changes to your health regimen.